Urinary Tract Infection
These are usually infections of the bladder and called cystitis. If a patient suffers repetitive urinary tract infections we may suggest some investigation in order to correctly diagnose the reason and offer appropriate treatments to assist recovery.
We may suggest ultrasounds to examine the kidneys or a CT which is an x-ray of the urinary tract to show function of the kidneys and ureters draining to the bladder. A cystoscopy may be necessary.
Recurrent UTI (Urinary Tract Infection)
Management of Recurrent Urinary Tract Infections
These are usually infections of the bladder and called cystitis and investigations of recurrent urinary tract infection.
Cystitis
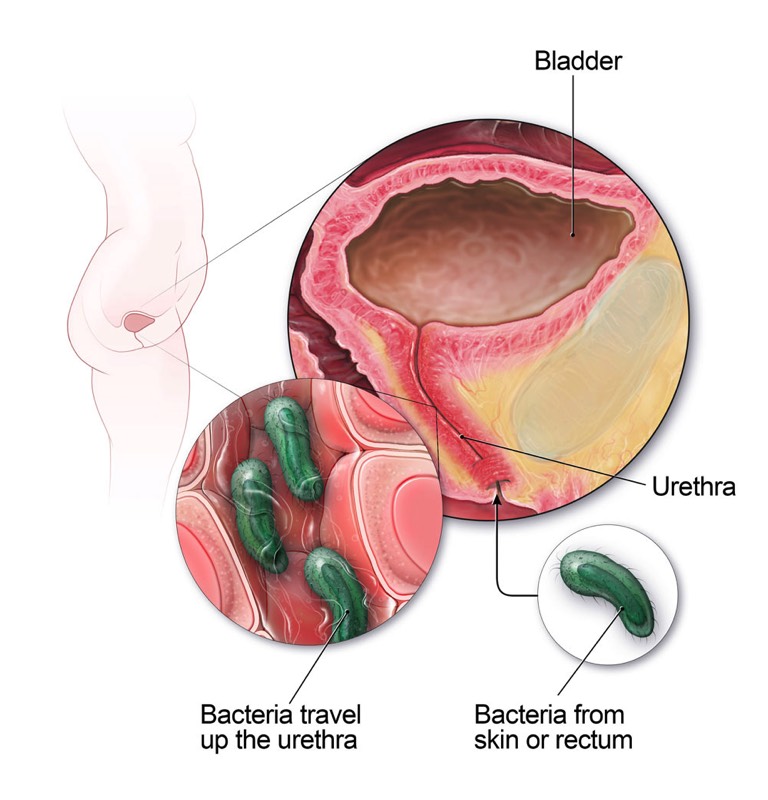
Urinary tract infection or cystitis is usually caused by a bacterial infection.
It is more common in females than in males because the urethra or pipe emptying the bladder is shorter in woman. Generally it is usually no longer than about 4.5 cm in the adult female.
The infecting organisms usually enter through the urethra and into the bladder giving symptoms of frequency of urination, burning and stinging upon urination and occasionally incontinence, bed wetting and blood in the urine. There may also be cramping lower abdominal pain.
The organisms get into the urethra from the surrounding tissues. A woman does not have to be dirty or lacking in hygiene to get a urinary infection. In sexually active women infection is sometimes massaged into the bladder through the actions of intercourse.
Patients who have had a catheter inserted into the bladder have an increased risk of urinary tract infections as a result of that being in place.
If bowels are not regular or there is diarrhoea on a recurrent basis then there is an increased chance of urinary tract infection.
In some female patients there is a reduction in the amount or quality of mucus which normally resists infection around the opening to the bladder. Sometimes that is the result of a hormonal abnormality.
Patients with diabetes have an increased chance of urinary tract infection.
Diagnosis
Urinary tract infection is usually diagnosed by finding bacteria in a mid stream urine (MSU) specimen. The specimen is collected by passing the initial amount of urine into the toilet, collecting the next 15-20mls or so in a sterile container and then passing the remainder down the toilet.
The specimen is then sent to the laboratory for examination under the microscope and to attempt to grow the abnormal organisms. That infection (growth) is then tested against antibiotics to see that the antibiotics will kill the bacteria. While the test is taking place which generally takes approximately 24 hours the Doctor usually writes a prescription for an antibiotic which is most likely the one that will clear up the infection. Treatment with antibiotics generally ranges from 1 to 5 days.
Investigations
1 CT Urogram which is an x-ray examination of the urinary tract in which an injection is given into a vein so that the function of the kidneys is shown up by passage of the dye through the kidneys and down the tubes (ureters) draining them to the bladder. This demonstrates the function and shows up delay in emptying and drainage of the kidneys and bladder.
2 Ultrasound which will show up the size and position of the kidneys and if there are any lumps or cysts associated with them. It will show if there is any dilation (widening) of the tubes which may be the result of blockage. It is also used to measure how much urine is in the bladder before and after going to the toilet. It does not show how well the kidneys function.
3 Cystoscopy. The cystoscope is an endoscopic instrument which is passed into the bladder through the normal passage (urethra) in order to inspect its lining. This procedure may either be carried out under local anaesthetic or general anaesthetic (when the patient is asleep) Read more…
Reducing the Frequency and Incidence of Urinary Tract Infection
1. Fluid Intake
Generally speaking an adult requires an intake of 2-3 litres of liquid per day in order to maintain adequate hydration and good urinary output.
Some substances such as alcohol and the caffeine containing drinks (tea, coffee and cola drinks) can cause significant bladder irritation.
After emptying the bladder the urethra should be wiped from front to back and never in the opposite direction. It is incorrect to rub as if drying with a towel as that will cause further irritation.
The genital region should be washed at the time of a bath or shower in the same direction (front to back) and may be washed gently with soap and water without adverse consequences. Occasionally some patients are sensitive to perfumed soaps which can cause irritation and they should be avoided. All soap should be washed away. It is good idea to wash morning and night. Hands should be washed before and after cleaning the genital area and after going to the toilet.
Clean underwear should be worn each day and should not be worn at night to allow air circulation to take place.
2. Bowels
It is important to maintain a good regular bowel habit and a high fibre diet is encouraged. A good (>2 litres per 24 hours) intake of fluid should accompany a high fibre diet.
3. Intercourse
The bladder should be emptied at a reasonable interval after having intercourse and a glass of water (approximately 400mls minimum) should be consumed. This assists with flushing the bladder out to help keep it clean.
4. Urinary Alkalinisers
Medications such as Ural® or Citravescent® change the pH of the urine from acid to alkaline. This has the effect of reducing stinging and irritation at the time of urination.
5. Antibiotics and Antiseptics
Occasionally a patient is prescribed antibiotics or antiseptics for a prolonged period of time which is usually a number of weeks or months. This is designed to assist in reducing the number of urinary tract infections occurring. Occasionally a breakthrough or resisstant infection can occur despite the use of these low dose antibiotics. This may occur for a number of reasons such as failure of the above management or the development of antibiotic resistant organisms. That will normally be detected on the MSU and the appropriate antibiotic will then be given.
6. Hormones
Often deficiency of oestrogen is replaced by using a cream which is applied to the vulval (external genital) area around the urethra and close to the opening of the vagina and its front wall in a sparing fashion each night. This improves the health of the tissues, reduces irritation and increases resistance to infection. It may take a few weeks to start working (3-4) but may be continued for a lifetime unless there are medical reasons not to (e.g. certain gynaecological cancers). Very little of this is absorbed in to the body so side-effects are very unusual.
These are usually infections of the bladder and called cystitis. If a patient suffers repetitive urinary tract infections we may suggest some investigation in order to correctly diagnose the reason and offer appropriate treatments to assist recovery.
We may suggest ultrasounds to examine the kidneys or a CT which is an x-ray of the urinary tract to show function of the kidneys and ureters draining to the bladder. A cystoscopy may be necessary.
Recurrent UTI (Urinary Tract Infection)
Management of Recurrent Urinary Tract Infections
These are usually infections of the bladder and called cystitis and investigations of recurrent urinary tract infection.
Cystitis
Urinary tract infection or cystitis is usually caused by a bacterial infection.
It is more common in females than in males because the urethra or pipe emptying the bladder is shorter in woman. Generally it is usually no longer than about 4.5 cm in the adult female.
The infecting organisms usually enter through the urethra and into the bladder giving symptoms of frequency of urination, burning and stinging upon urination and occasionally incontinence, bed wetting and blood in the urine. There may also be cramping lower abdominal pain.
The organisms get into the urethra from the surrounding tissues. A woman does not have to be dirty or lacking in hygiene to get a urinary infection. In sexually active women infection is sometimes massaged into the bladder through the actions of intercourse.
Patients who have had a catheter inserted into the bladder have an increased risk of urinary tract infections as a result of that being in place.
If bowels are not regular or there is diarrhoea on a recurrent basis then there is an increased chance of urinary tract infection.
In some female patients there is a reduction in the amount or quality of mucus which normally resists infection around the opening to the bladder. Sometimes that is the result of a hormonal abnormality.
Patients with diabetes have an increased chance of urinary tract infection.
Diagnosis
Urinary tract infection is usually diagnosed by finding bacteria in a mid stream urine (MSU) specimen. The specimen is collected by passing the initial amount of urine into the toilet, collecting the next 15-20mls or so in a sterile container and then passing the remainder down the toilet.
The specimen is then sent to the laboratory for examination under the microscope and to attempt to grow the abnormal organisms. That infection (growth) is then tested against antibiotics to see that the antibiotics will kill the bacteria. While the test is taking place which generally takes approximately 24 hours the Doctor usually writes a prescription for an antibiotic which is most likely the one that will clear up the infection. Treatment with antibiotics generally ranges from 1 to 5 days.
Investigations
1 CT Urogram which is an x-ray examination of the urinary tract in which an injection is given into a vein so that the function of the kidneys is shown up by passage of the dye through the kidneys and down the tubes (ureters) draining them to the bladder. This demonstrates the function and shows up delay in emptying and drainage of the kidneys and bladder.
2 Ultrasound which will show up the size and position of the kidneys and if there are any lumps or cysts associated with them. It will show if there is any dilation (widening) of the tubes which may be the result of blockage. It is also used to measure how much urine is in the bladder before and after going to the toilet. It does not show how well the kidneys function.
3 Cystoscopy. The cystoscope is an endoscopic instrument which is passed into the bladder through the normal passage (urethra) in order to inspect its lining. This procedure may either be carried out under local anaesthetic or general anaesthetic (when the patient is asleep) Read more…
Reducing the Frequency and Incidence of Urinary Tract Infection
1. Fluid Intake
Generally speaking an adult requires an intake of 2-3 litres of liquid per day in order to maintain adequate hydration and good urinary output.
Some substances such as alcohol and the caffeine containing drinks (tea, coffee and cola drinks) can cause significant bladder irritation.
After emptying the bladder the urethra should be wiped from front to back and never in the opposite direction. It is incorrect to rub as if drying with a towel as that will cause further irritation.
The genital region should be washed at the time of a bath or shower in the same direction (front to back) and may be washed gently with soap and water without adverse consequences. Occasionally some patients are sensitive to perfumed soaps which can cause irritation and they should be avoided. All soap should be washed away. It is good idea to wash morning and night. Hands should be washed before and after cleaning the genital area and after going to the toilet.
Clean underwear should be worn each day and should not be worn at night to allow air circulation to take place.
2. Bowels
It is important to maintain a good regular bowel habit and a high fibre diet is encouraged. A good (>2 litres per 24 hours) intake of fluid should accompany a high fibre diet.
3. Intercourse
The bladder should be emptied at a reasonable interval after having intercourse and a glass of water (approximately 400mls minimum) should be consumed. This assists with flushing the bladder out to help keep it clean.
4. Urinary Alkalinisers
Medications such as Ural® or Citravescent® change the pH of the urine from acid to alkaline. This has the effect of reducing stinging and irritation at the time of urination.
5. Antibiotics and Antiseptics
Occasionally a patient is prescribed antibiotics or antiseptics for a prolonged period of time which is usually a number of weeks or months. This is designed to assist in reducing the number of urinary tract infections occurring. Occasionally a breakthrough or resisstant infection can occur despite the use of these low dose antibiotics. This may occur for a number of reasons such as failure of the above management or the development of antibiotic resistant organisms. That will normally be detected on the MSU and the appropriate antibiotic will then be given.
6. Hormones
Often deficiency of oestrogen is replaced by using a cream which is applied to the vulval (external genital) area around the urethra and close to the opening of the vagina and its front wall in a sparing fashion each night. This improves the health of the tissues, reduces irritation and increases resistance to infection. It may take a few weeks to start working (3-4) but may be continued for a lifetime unless there are medical reasons not to (e.g. certain gynaecological cancers). Very little of this is absorbed in to the body so side-effects are very unusual.
