
The Bladder
The bladder is a muscular sac which retains and stores urine, a waste by-product from cell respiration. Urine accumulates until it is expelled from the body via the urethra - a tube connecting the bladder with the exterior; this runs through the penis in men. A sphincter controls the flow of urine out of the bladder.
Incontinence
Urinary Incontinence
Incontinence is the inability to voluntarily control urination. It may be a result of an inability of the bladder to hold urine or a deficiency in strength of the Distal Urethral Sphincter (DUS) or a combination.
There are several types of incontinence which present requiring treatment:
1. Urge incontinence – this occurs when the patient has the urge to go to the toilet and leaks before getting there.
2. Stress incontinence – leakage with a laugh, cough or sneeze, usually only a small amount.
3. Combination – the cough, laugh or sneeze or pressure increase in the abdomen leads to stimulation of a bladder contraction and more than a drop leaks out.
4. Total incontinence where there is continuous leakage. This may be the result of an abnormal opening or "hole" or may be overflow where the bladder fills up and leaks out like a reservoir spillway.
Urodynamics
Urodynamics is the study of the bladder's ability to hold urine and empty it in a normal fashion.
It is carried out on both male and female patients.
If you are undergoing Urodynamic studies it is likely that you have some of the following symptoms:
• Discomfort of passing urine;
• Urgency of urination where you have to hurry to the toilet;
• Stress incontinence where urine leaks out with cough, laugh or sneeze;
• Complete incontinence where the urine leaks all the time;
• A decrease in the flow of urination;
• A decrease in the ability to stop urinating;
• Irregular urination;
• Bedwetting.
Cystoscopy
The procedure is carried out in order to obtain a diagnosis for patients with symptoms such as recurrent infection, pain, bleeding, difficult or frequent urination.
Cystoscopy is a procedure which is carried out using an endoscopic instrument to visualise the lower urinary tract which includes the bladder and the urethra (pipe draining the urine to the outside).
Cystoscopy is usually carried out as a day surgical procedure and generally speaking admission to hospital overnight is not required. Admission may be required if some further procedures are found necessary at the time which need in-hospital care. This is very unusual. The need for admission will be discussed with the patient the procedure has been completed. This is necessary in less than 1 in 3000 patients.
The procedure is usually carried out under a general anaesthetic with a rigid instrument. That is, the patient is completely asleep. Sometimes the procedure may be carried out under regional anaesthesia where the patient is given an injection into a vein to induce drowsiness and another injection is placed in the patient’s back so there is no feeling or pain below the waist. Alternatively if it is proposed to carry out a Flexible Cystoscopy, the patient is usually wide awake with no sedation and a local anaesthetic jelly is injected down the urethra in order to reduce sensation. This is done without the use of a needle.
The advantage of Flexible Cystoscopy is that fasting is not needed and sedation or anaesthesia (regional or general) is not needed. The disadvantage of Flexible Cystoscopy is that if there is a lesion present which might require removal or biopsy (sampling) then that may not be possible to be carried out using the flexible cystoscope and it may be necessary for the patient to return at a later date and have a general anaesthetic in order for the lesion to be removed with a similar rigid instrument. If with a routine cystoscopy (rigid), a lesion is seen then all efforts are made to completely remove that at the time of the procedure. This is usually referred to as a transurethral resection. If the patient is a male and the problem is enlargement of the prostate, a prostate operation will NOT be carried out at that time. The proposed procedure will be discussed with the patient prior to proceeding at a later date.
If it is necessary to remove tissue, then there will be an additional charge for that procedure and the patient will receive an account from the Pathologist to whom it has been sent for examination.
Admission to Hospital
The patient must bring all medications to hospital at the time of admission. No medications should be ceased unless the patient is instructed to do so by the Doctor.
Before Theatre
The admitting nurse will take down the patient’s history and prepare the patient for theatre. This may include:
• Collecting a sample of urine before the procedure
• A shower with careful attention to the genital area
N.B. soap only, no powder or deodorant
It will include:
• Dressed in theatre attire
• Consultation by the Anaesthetist and pre-med given if ordered
• Nursing staff will escort the patient to theatre
• The patient will continue to remain fasting until after the operation which means nothing to eat or drink, including lollies and chewing gum.
• Please do not smoke prior to the anaesthetic
Generally speaking the patient will fast for 4-6 hours pre-operatively which means no intake of anything whatsoever including water.
After the Operation
When the operation is over, the patient will spend a short time in the recovery room. The nurses will monitor the patient closely until awake or the patient regains feeling in the legs (if a spinal anaesthetic).
The staff will take the pulse, blood pressure and temperature regularly for the first couple of hours. This is routine.
There may be an IV (drip) in place which is providing liquid until the patient is able to drink normally.
There may be some bleeding in the urine but it is usually of small amounts as a result of the manipulation and will settle spontaneously with a good fluid throughput.
Occasionally there is some discomfort on passing urine and this may be helped by Ural or Citravscent.
The patient will be reviewed prior to being discharged from Day Surgery and the findings, diagnosis and proposed plan of management outlined. It is often a good for a carer who is driving the patient home to be present at that time in order that some drowsiness associated with the anaesthetic does not affect understanding.
An appointment for review at the consulting rooms will be made prior to the patient’s discharge.
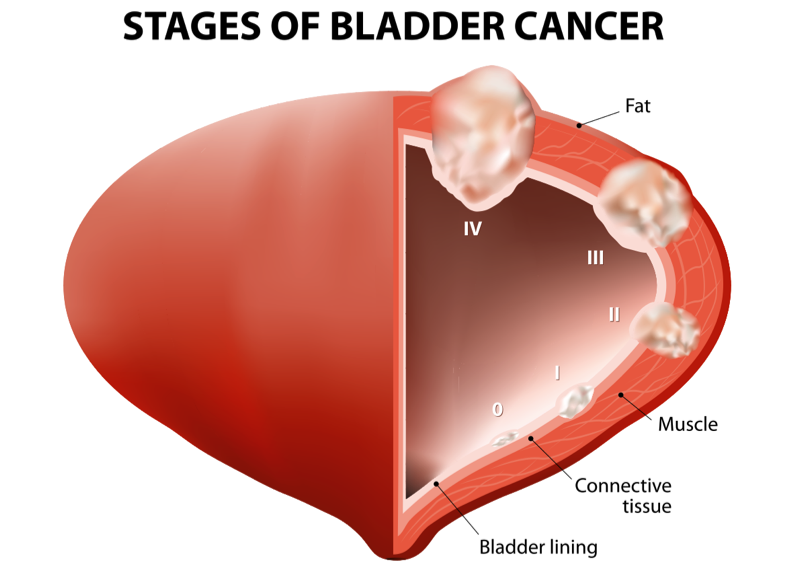
Bladder Tumour
Bladder tumours are growths which arise from the lining of the bladder and usually present when they bleed leading to the patient seeking advice because of blood in the urine.
A CT Urogram is an x-ray of the lining of the kidneys and bladder which is usually carried out to see if there is any possible source of bleeding from the kidneys and the ureters (tubes) which drain the urine into the bladder.
Ultrasounds are often done to check the solid part of the kidneys.
Occasionally a tumour may be small as to not be detected by these tests.
Although it is more common for tumours to develop in the bladder itself, the X-ray is necessary because the same type of skin lines the kidneys and ureters as lines the bladder.
In order to diagnose a bladder tumour it is necessary to have a cystoscopic examination of the bladder.
read more…..
The bladder is a muscular sac which retains and stores urine, a waste by-product from cell respiration. Urine accumulates until it is expelled from the body via the urethra - a tube connecting the bladder with the exterior; this runs through the penis in men. A sphincter controls the flow of urine out of the bladder.
Incontinence
Urinary Incontinence
Incontinence is the inability to voluntarily control urination. It may be a result of an inability of the bladder to hold urine or a deficiency in strength of the Distal Urethral Sphincter (DUS) or a combination.
There are several types of incontinence which present requiring treatment:
1. Urge incontinence – this occurs when the patient has the urge to go to the toilet and leaks before getting there.
2. Stress incontinence – leakage with a laugh, cough or sneeze, usually only a small amount.
3. Combination – the cough, laugh or sneeze or pressure increase in the abdomen leads to stimulation of a bladder contraction and more than a drop leaks out.
4. Total incontinence where there is continuous leakage. This may be the result of an abnormal opening or "hole" or may be overflow where the bladder fills up and leaks out like a reservoir spillway.
Urodynamics
Urodynamics is the study of the bladder's ability to hold urine and empty it in a normal fashion.
It is carried out on both male and female patients.
If you are undergoing Urodynamic studies it is likely that you have some of the following symptoms:
• Discomfort of passing urine;
• Urgency of urination where you have to hurry to the toilet;
• Stress incontinence where urine leaks out with cough, laugh or sneeze;
• Complete incontinence where the urine leaks all the time;
• A decrease in the flow of urination;
• A decrease in the ability to stop urinating;
• Irregular urination;
• Bedwetting.
Cystoscopy
The procedure is carried out in order to obtain a diagnosis for patients with symptoms such as recurrent infection, pain, bleeding, difficult or frequent urination.
Cystoscopy is a procedure which is carried out using an endoscopic instrument to visualise the lower urinary tract which includes the bladder and the urethra (pipe draining the urine to the outside).
Cystoscopy is usually carried out as a day surgical procedure and generally speaking admission to hospital overnight is not required. Admission may be required if some further procedures are found necessary at the time which need in-hospital care. This is very unusual. The need for admission will be discussed with the patient the procedure has been completed. This is necessary in less than 1 in 3000 patients.
The procedure is usually carried out under a general anaesthetic with a rigid instrument. That is, the patient is completely asleep. Sometimes the procedure may be carried out under regional anaesthesia where the patient is given an injection into a vein to induce drowsiness and another injection is placed in the patient’s back so there is no feeling or pain below the waist. Alternatively if it is proposed to carry out a Flexible Cystoscopy, the patient is usually wide awake with no sedation and a local anaesthetic jelly is injected down the urethra in order to reduce sensation. This is done without the use of a needle.
The advantage of Flexible Cystoscopy is that fasting is not needed and sedation or anaesthesia (regional or general) is not needed. The disadvantage of Flexible Cystoscopy is that if there is a lesion present which might require removal or biopsy (sampling) then that may not be possible to be carried out using the flexible cystoscope and it may be necessary for the patient to return at a later date and have a general anaesthetic in order for the lesion to be removed with a similar rigid instrument. If with a routine cystoscopy (rigid), a lesion is seen then all efforts are made to completely remove that at the time of the procedure. This is usually referred to as a transurethral resection. If the patient is a male and the problem is enlargement of the prostate, a prostate operation will NOT be carried out at that time. The proposed procedure will be discussed with the patient prior to proceeding at a later date.
If it is necessary to remove tissue, then there will be an additional charge for that procedure and the patient will receive an account from the Pathologist to whom it has been sent for examination.
Admission to Hospital
The patient must bring all medications to hospital at the time of admission. No medications should be ceased unless the patient is instructed to do so by the Doctor.
Before Theatre
The admitting nurse will take down the patient’s history and prepare the patient for theatre. This may include:
• Collecting a sample of urine before the procedure
• A shower with careful attention to the genital area
N.B. soap only, no powder or deodorant
It will include:
• Dressed in theatre attire
• Consultation by the Anaesthetist and pre-med given if ordered
• Nursing staff will escort the patient to theatre
• The patient will continue to remain fasting until after the operation which means nothing to eat or drink, including lollies and chewing gum.
• Please do not smoke prior to the anaesthetic
Generally speaking the patient will fast for 4-6 hours pre-operatively which means no intake of anything whatsoever including water.
After the Operation
When the operation is over, the patient will spend a short time in the recovery room. The nurses will monitor the patient closely until awake or the patient regains feeling in the legs (if a spinal anaesthetic).
The staff will take the pulse, blood pressure and temperature regularly for the first couple of hours. This is routine.
There may be an IV (drip) in place which is providing liquid until the patient is able to drink normally.
There may be some bleeding in the urine but it is usually of small amounts as a result of the manipulation and will settle spontaneously with a good fluid throughput.
Occasionally there is some discomfort on passing urine and this may be helped by Ural or Citravscent.
The patient will be reviewed prior to being discharged from Day Surgery and the findings, diagnosis and proposed plan of management outlined. It is often a good for a carer who is driving the patient home to be present at that time in order that some drowsiness associated with the anaesthetic does not affect understanding.
An appointment for review at the consulting rooms will be made prior to the patient’s discharge.
Bladder Tumour
Bladder tumours are growths which arise from the lining of the bladder and usually present when they bleed leading to the patient seeking advice because of blood in the urine.
A CT Urogram is an x-ray of the lining of the kidneys and bladder which is usually carried out to see if there is any possible source of bleeding from the kidneys and the ureters (tubes) which drain the urine into the bladder.
Ultrasounds are often done to check the solid part of the kidneys.
Occasionally a tumour may be small as to not be detected by these tests.
Although it is more common for tumours to develop in the bladder itself, the X-ray is necessary because the same type of skin lines the kidneys and ureters as lines the bladder.
In order to diagnose a bladder tumour it is necessary to have a cystoscopic examination of the bladder.
read more…..
BCG Treatment
BCG is the same substance used for vaccinating patients against tuberculosis (TB). It has been found that when this substance is placed into the bladder, it causes the body to make cells which then attack the cancer cells. This is known as immunotherapy. In other words it is teaching the body to recognise the cancerous cells as being abnormal and to engulf and destroy them. It does not work in every case and may have some side effects.
read more…..
Bladder Stones
Bladder stones are usually associated with an enlarged prostate but sometimes also occur in female patients. Most bladder stones can be removed with endoscopic instruments passed through the urethra. They usually need to be broken up with a mechanical instrument or Laser first. Some are too large. For example, >5cm and are more easily removed with "open surgery" where a small incision is made on the lower abdomen and the stone lifted out The wound is closed with sutures.The patient will have a catheter in place for approximately one week after the operation to help the bladder to heal.
read more
BCG is the same substance used for vaccinating patients against tuberculosis (TB). It has been found that when this substance is placed into the bladder, it causes the body to make cells which then attack the cancer cells. This is known as immunotherapy. In other words it is teaching the body to recognise the cancerous cells as being abnormal and to engulf and destroy them. It does not work in every case and may have some side effects.
read more…..
Bladder Stones
Bladder stones are usually associated with an enlarged prostate but sometimes also occur in female patients. Most bladder stones can be removed with endoscopic instruments passed through the urethra. They usually need to be broken up with a mechanical instrument or Laser first. Some are too large. For example, >5cm and are more easily removed with "open surgery" where a small incision is made on the lower abdomen and the stone lifted out The wound is closed with sutures.The patient will have a catheter in place for approximately one week after the operation to help the bladder to heal.
read more
